By Rebecca Thornton and Ariella Park
Voluntary medical male circumcision (VMMC) is a key component of the HIV prevention strategy recommended by the
World Health Organization (PDF) in fourteen priority African countries with high HIV prevalence rates. Simulated projections by
Njeuhmeli et al. in 2011 suggested that reaching 80 percent VMMC coverage in these countries by 2015 could result in net savings of more than US$16 billion and avert more than 3 million HIV infections over fifteen years.
However, the
WHO reported (PDF) in July that priority countries had only reached 44 percent VMMC coverage. While some countries exceeded their targets, others lagged far behind—Malawi, for example, had only reached 8 percent of its target coverage levels. What might explain this slow progress? And, more importantly, what can be done to increase circumcision rates?
A new
J-PAL policy briefcase (PDF) summarizes results from two randomized evaluations conducted in Malawi, with Susan Godlonton and other co-authors. It provides insight into the central problem of low demand in this context. These studies were the first to measure the demand for VMMC through population-based surveys, which hint at even lower levels of demand than previously suggested by clinical statistics or popular media.
In 2008, an evaluation measured the
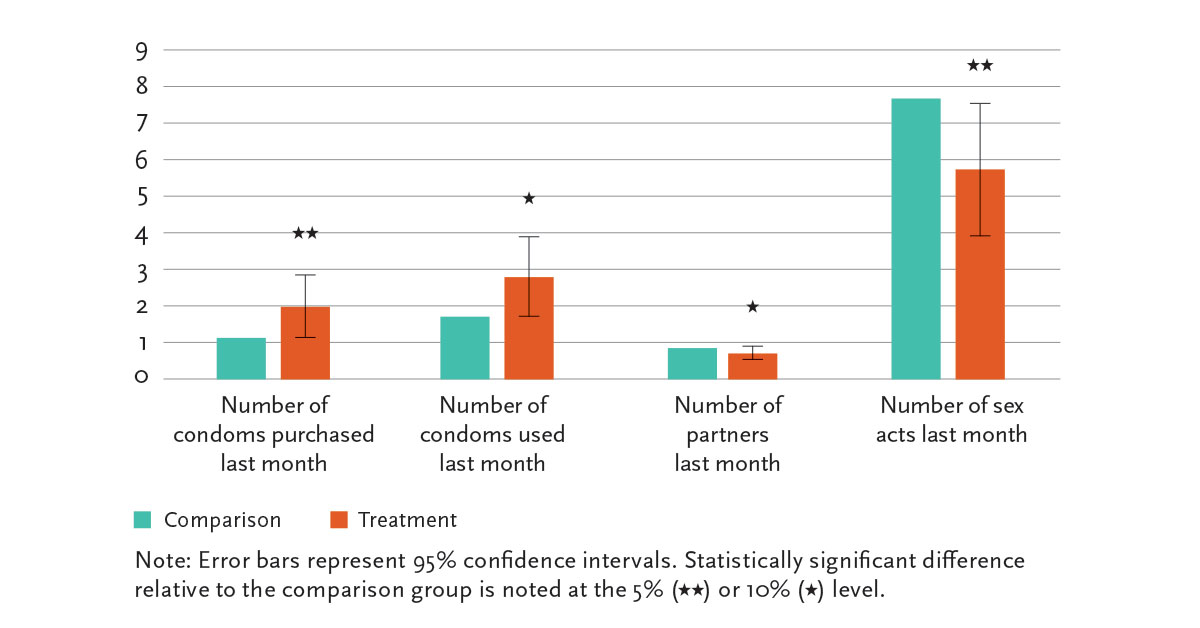
impact of a VMMC information campaign on adult men in a rural area of Southern Malawi. One year after receiving the information, uncircumcised men were less likely to engage in risky sexual behavior—however the information had no impact on VMMC take-up, with only 2% of men getting a circumcision.
In 2010, a second evaluation in urban Lilongwe found take-up of circumcision was
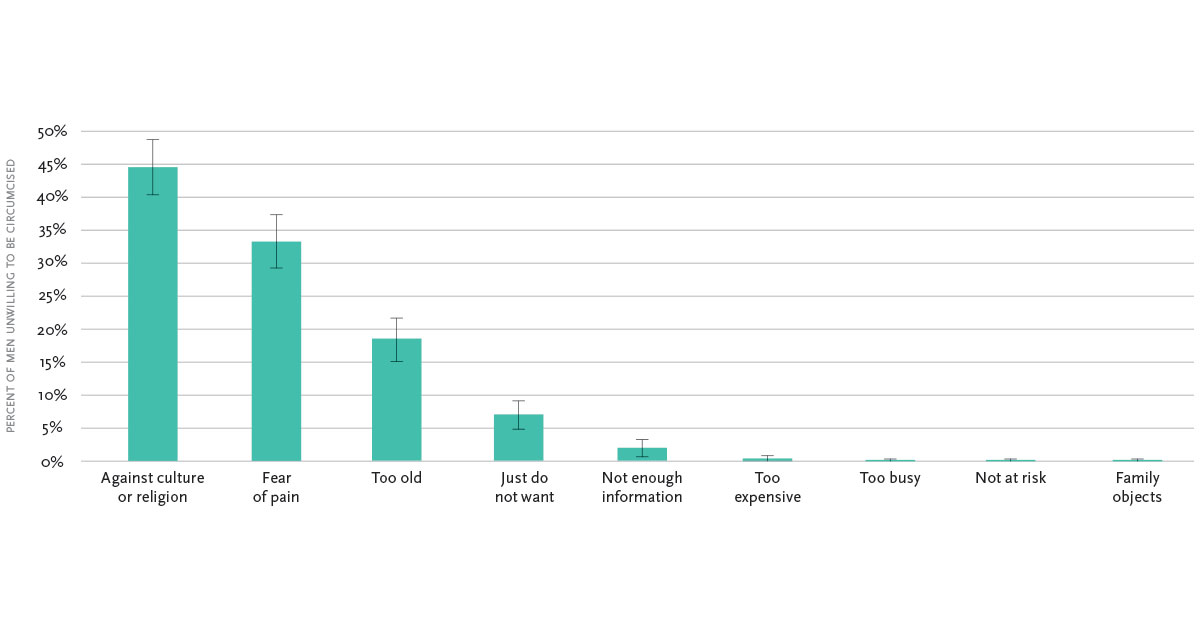
similarly low, at only 3%. In addition, providing information or lowering the price of VMMC only slightly increased take-up. Follow-up surveys one year later showed that information and price had little impact on the most commonly cited reasons for being unwilling to be circumcised: cultural or religious reasons and fear of pain.
The low demand found in both studies could offer one explanation for why progress towards the targeted 80 percent coverage has been slow in Malawi. While price and information matter, other barriers are more important in this context. Our two studies in Malawi demonstrate the critical importance of future research on interventions in low-demand contexts that effectively address barriers such as cultural norms and fear of pain.
Much promising work has already been done in this space. For example--3ie has funded seven impact evaluations on demand creation for VMMC; preliminary results were presented earlier this month at the International Conference on AIDS and STIs in Africa, in Zimbabwe. Another recent study published in JAMA by Harsha Thirumurthy et al., examined the impact of providing food vouchers for men in Kenya to receive circumcisions.
Rebecca Thornton is an IPA research network member and Associate Professor of economics and the University of Illinois at Urbana Champaign, Ariella Park is a policy associate at J-PAL.
Paper Citations:
Chinkhumba, Jobiba, Susan Godlonton, and Rebecca Thornton. 2014. “The Demand for Medical Male Circumcision.” American Economic Journal: Applied Economics 6(2):152–177.
Godlonton, Susan, Alister Munthali, and Rebecca Thornton. “Responding to Risk: Circumcision, Information, and HIV Prevention.” The Review of Economics and Statistics, forthcoming.
Maughan-Brown, Brendan, Susan Godlonton, Rebecca Thornton, and Atheendar S. Venkataraman. 2015. “What Do People Actually Learn from Public Health Campaigns? Incorrect Inferences about Male Circumcision and Female HIV Infection Risk Among Men and Women in Malawi.” AIDS and Behavior 19:1170–1177.